Acne frustrates teenagers and adults alike. It appears suddenly. It lingers. It often leaves marks behind.
You may blame chocolate. You may blame stress. You may blame dirty skin.
Let’s clear that up.
Acne forms through a chain reaction inside your pores. When you understand that chain, you stop guessing and start making smarter choices.
Here is why acne develops and what drives it…
First, Understand Your Pores
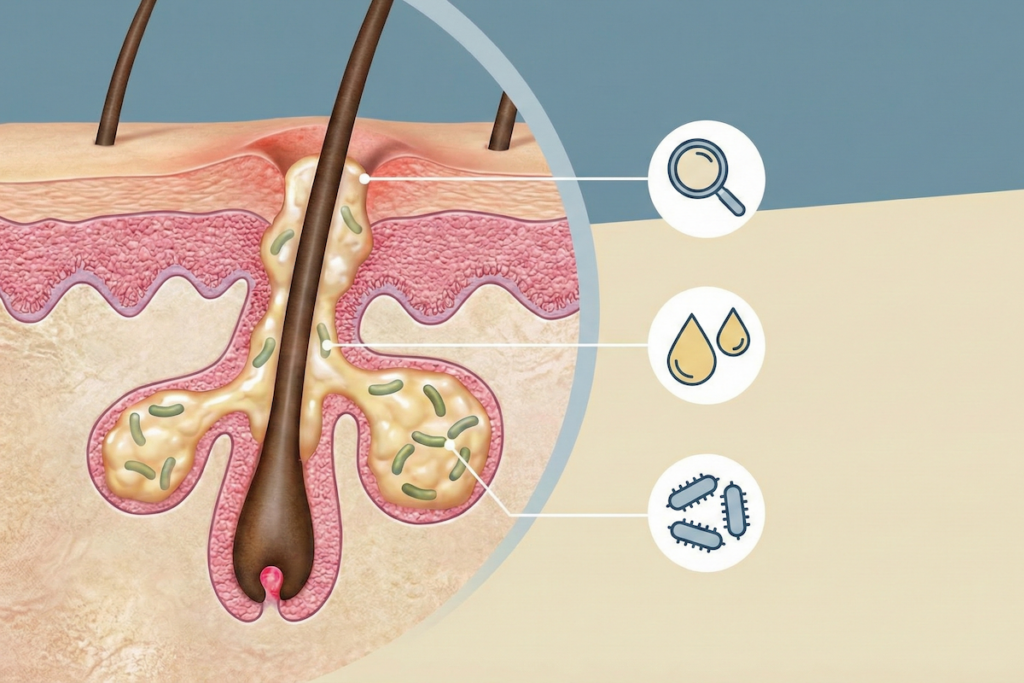
Your skin contains thousands of tiny openings called pores. Each pore connects to a hair follicle and an oil gland.
Oil glands produce sebum. Sebum lubricates your skin. It keeps your barrier soft and flexible.
When this system runs smoothly, your skin stays clear.
When it clogs, acne begins.
Let’s break the process into four steps.
The Four Main Causes of Acne
Dermatologists identify four core factors:
- Excess oil production
- Dead skin buildup
- Bacteria growth
- Inflammation
All four interact inside the pore.
Remove one factor and acne improves. Trigger several at once and breakouts increase.
1. Excess Oil Production
Oil, also called sebum, plays a protective role. Trouble starts when your glands produce too much.
Hormones often drive this increase.
During puberty, androgen hormones rise. These hormones stimulate oil glands. More oil means more opportunity for clogged pores.
Adults also experience hormonal shifts. Menstrual cycles, pregnancy, and stress affect oil levels.
Extra oil alone does not cause acne. It creates the right environment for blockage.
2. Dead Skin Cell Buildup
Your skin constantly renews itself. Old cells shed. New cells rise.
When shedding slows down, dead cells stick together inside the pore.
Oil mixes with these cells. The mixture thickens. The pore narrows.
Now you have a plug forming.
This plug can stay under the surface or reach the opening of the pore.
If the top remains closed, you see a whitehead.
If it opens and oxidizes, you see a blackhead.
That explains comedones.
But acne does not stop there.
3. Bacteria Growth
Your skin hosts bacteria naturally. One type, Cutibacterium acnes, lives deep inside pores.
When a pore clogs, oxygen levels drop. That environment suits bacteria. They multiply quickly.
As bacteria grow, your immune system responds. It sends white blood cells to fight the invasion.
This immune response triggers redness and swelling.
Now you see an inflamed pimple.
4. Inflammation
Inflammation defines the difference between a mild clogged pore and a painful cyst.
When your immune system reacts strongly, the pore wall can rupture. Oil and bacteria spill into surrounding tissue.
That causes:
- Red bumps
- Pustules
- Deep nodules
- Cysts
Inflammation determines severity.
Some people produce stronger inflammatory responses than others. Genetics influence this.
Types of Acne Lesions
Understanding lesion types helps you identify your pattern.
Whiteheads
Closed clogged pores. Small and flesh colored.
Blackheads
Open clogged pores. Dark surface from oxidation.
Papules
Small red bumps. Tender but without visible pus.
Pustules
Red bumps with white or yellow center.
Nodules
Large, painful, deep lumps.
Cysts
Deep, swollen, often painful lesions that can scar.
Mild acne involves mostly whiteheads and blackheads. Severe acne includes nodules and cysts.
What Triggers Acne?
Now that you know the mechanism, let’s look at triggers.
Triggers activate one or more of the four causes…
Hormones
Hormones increase oil production.
Puberty remains the most common trigger. Androgens stimulate sebaceous glands.
Women may notice breakouts:
- Before their period
- During pregnancy
- After stopping birth control
Hormonal acne often appears on the lower face and jawline.
If breakouts follow a monthly pattern, hormones likely play a role.
Genetics
If your parents had acne, you have higher odds of developing it.
Genes influence:
- Skin type
- Oil production
- Inflammatory response
- Pore structure
You cannot change genetics. You can manage symptoms.
Stress
Stress raises cortisol levels. Cortisol can stimulate oil production.
Stress also slows wound healing. That means breakouts linger longer.
You may notice flare ups during exams, deadlines, or emotional strain.
The connection is real.
Diet
Research continues to examine diet and acne.
High glycemic foods may spike insulin. Increased insulin can stimulate oil glands.
Dairy may influence hormones in some individuals.
Not everyone reacts the same way. Keep track of patterns. If breakouts follow certain foods consistently, take note.
Avoid extreme restrictions without evidence.
Skincare Habits
Harsh scrubbing irritates skin. Irritation increases inflammation.
Heavy pore clogging products trap oil and dead cells.
Sleeping in makeup blocks pores overnight.
Simple habits matter.
Friction and Pressure
Tight helmets, chin straps, and phone screens create friction. That pressure irritates follicles.
This type of breakout is called acne mechanica.
Athletes often experience it.
Medications
Certain medications increase acne risk, including:
- Corticosteroids
- Some birth control types
- Lithium
If acne appears after starting a new medication, speak with your doctor.
Why Washing More Does Not Cure Acne
Many people think acne equals dirty skin.
That belief leads to over washing.
Over cleansing strips your barrier. Your skin compensates by producing more oil. Inflammation increases.
Acne forms below the surface. Surface dirt does not cause it.
Gentle cleansing works better than scrubbing.
Acne in Adults
Adult acne continues into the 30s, 40s, and beyond.
Common reasons include:
- Hormonal shifts
- Stress
- Barrier damage from aggressive routines
- Certain cosmetic ingredients
Adult skin often feels drier than teenage skin. That changes treatment strategy.
Balance becomes the goal.
When Acne Leads to Scars
Inflammation damages surrounding tissue. Deep cysts increase scar risk.
Picking pimples raises the risk further. Squeezing pushes debris deeper into skin.
Scars form when collagen breaks down during healing.
Early management reduces long term marks.
Acne vs Other Skin Conditions
Not every bump equals acne.
Rosacea causes redness and bumps but follows a different pattern.
Folliculitis results from infected hair follicles.
Perioral dermatitis appears around the mouth.
If your condition does not respond to acne treatments, get evaluated.
Correct diagnosis matters.
The Role of the Skin Barrier
A damaged barrier worsens acne.
When your barrier weakens, inflammation rises. Irritation increases oil production.
Overuse of active ingredients often causes this.
Calm skin breaks out less.
Can Acne Be Prevented?
You cannot eliminate every breakout. You can reduce frequency.
Focus on:
- Gentle cleansing
- Avoiding pore clogging ingredients
- Managing stress
- Monitoring hormonal patterns
- Protecting the barrier
Consistency works better than aggression.
When to See a Dermatologist
Seek help if you experience:
- Painful cysts
- Scarring
- Acne that does not improve
- Emotional distress related to breakouts
Prescription treatments target oil, bacteria, and inflammation at deeper levels.
You do not need to suffer in silence.
Let’s Pull It Together
Acne forms when oil, dead skin cells, bacteria, and inflammation collide inside a pore.
Triggers like hormones, stress, and certain habits activate that process.
Acne does not mean you are dirty. It does not mean you failed at skincare.
It means your pores clogged and your immune system reacted.
Next steps:
Observe your breakout pattern.
Notice timing.
Avoid harsh stripping.
Support your skin barrier.
Understanding the cause gives you control.